Buyers Guide
Oxygen Concentrators for Supplemental Oxygen Therapy
Why are Oxygen Concentrators Important for Healthcare Settings?
There are 3 main sources for oxygen in most health care settings: (1) piped oxygen systems which are typically at higher level facilities with more resources and patient volume; (2) oxygen cylinders, which do not require electricity but do require other accessories to deliver the oxygen to patients; and (3) oxygen concentrators, which are self-contained medical devices, electrically powered, that concentrate oxygen from the ambient air. There are a number of factors to consider depending on the oxygen source, the upfront cost and lifespan of the product, but also operating costs that might include spare parts, accessories, purchasing or leasing agreements, and shipping and installation costs.
This buyers guide will specifically cover Oxygen Concentrators. (For additional information and guidance about supplemental oxygen therapy and related products; VIA recommends this resource: WHO-UNICEF Technical Specifications and Guidance for Oxygen Therapy Products, 2019)
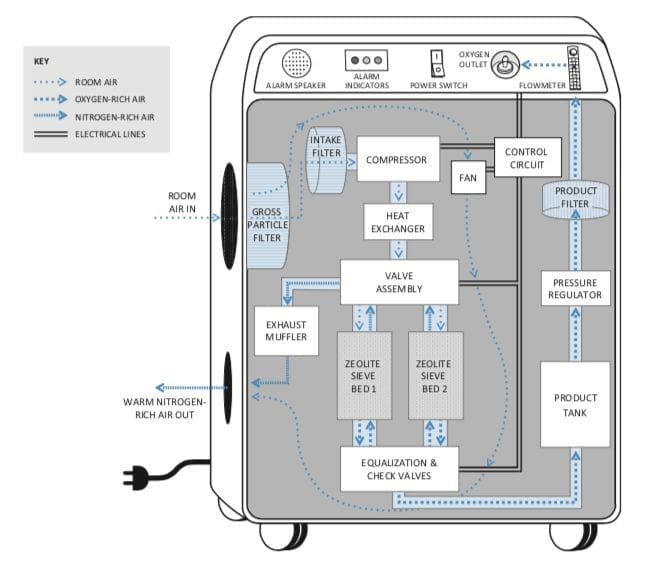
Benefits of Oxygen Concentrators. Oxygen concentrators can play an important role in improving quality of care and increasing access to life-saving oxygen, even in lower-resource settings. If used correctly and maintained adequately, they also have the advantage of being more reliable and lower-cost compared to piped oxygen systems and oxygen cylinders. As a source of oxygen for delivering supplemental oxygen to treat hypoxia, oxygen concentrators have an advantage of being able to process ambient air into the appropriate amount of oxygen that patients require for their clinical condition.
These devices also can manage the “flow rate” based on patient size, clinical requirements, and the interface, or delivery mode. Another benefit of oxygen concentrators is that they can provide a continuous supply of oxygen to multiple patients at the same time when used with a flowsplitter or flowmeter stand for splitting. (see related Buyers Guide for Oxygen Accessories). The percent oxygen a patient will receive depends on the mode of delivery to the patient and their clinical needs (i.e., nasal prongs, nasal catheter, facemask, etc.).
Types of Oxygen Concentrators
Oxygen concentrators are either stationary or portable
Stationary Oxygen Concentrators are self-contained devices that supply a continuous stream of oxygen at flow rates up to 10 L/min; or very low flow rates as low as 0.1 L/min with the assistance of an integrated flowmeter or additional accessories. Most concentrators should deliver at least 5 L/min and operate on AC electricity, consuming 280-600 watts depending on the model. However, many manufacturers offer models or adapters to match the local power grid.
Portable Oxygen Concentrators have a lower flow capacity (<3 L/min), consume less power than stationary concentrators, and are more commonly used by individual patients and not suitable for multiple patients. Furthermore, some portable oxygen concentrators restrict oxygen delivery during inspiration. This intermittent flow, while it conserves oxygen and battery power, is not appropriate for neonates and children who may not be able to generate enough negative pressure during inspiration to trigger the flow of oxygen.
UNICEF has developed an Excel-based tool for healthcare facilities and procurement officials to plan for their oxygen needs, from source to delivery and understand what solutions might be available to increase their oxygen availability.
What are Key Considerations for Selecting an Oxygen Concentrator?
- Oxygen Concentration (or purity). Oxygen concentrators should deliver a continuous flow of oxygen at concentration of 82%-96%, and have an alarm or indicator when concentration is producing lower than 82% concentration.
- Flow control. The device should be equipped with at least one flowmeter that can control flow-rate. If there are more flowmeters, each needs its own flow-rate control. The oxygen concentrators should also be prevented from providing a flow rate EXCEEDING the maximum rated flow rate, for safety purposes. (See Buyers Guide for Oxygen Accessories)
- Humidification. Depending on clinical use and patient, humidification might be important. Some concentrators come with humidification bottles. See below for special considerations for neonates.
- Cost. Oxygen concentrators can range widely in cost, but customers should also consider the initial costs of spare parts, installation, accessories, and training of health care personnel in appropriate use and maintenance. Ongoing operational costs are generally limited to electricity and maintenance, but may vary depending on power availability and the clinical use.
- Power. Concentrators require a source of reliable and continuous power to function safely and effectively. For facilities where this is a constraint, having an independent oxygen source, such as a cylinder, is crucial. In addition to having electrical plugs that are compatible with the power outlets of the designated facility, concentrators should also have power efficiency of < 70 W/LPM.
- Outlets. Devices should have at least one outlet for attachment of oxygen delivery tubing. If these outlets protrude or are made of flimsy materials, the likelihood of damage or breakage is higher. Barbed fittings and recessed outlets are good designs to prevent tubing misconnections.
- User Care. Preventive maintenance of oxygen concentrators should include cleaning of filters and preventive and periodic maintenance to ensure oxygen output. Some concentrators may have more detailed instructions on preventive maintenance, or built in alarms and alerts.
- Performance in lower-resource settings. Factors such as extreme temperatures and humidity, or unstable power sources can present operational challenges to oxygen concentrators. Appropriate and adequate training of technicians or engineers is important to provide preventive and corrective maintenance to prevent device failure.
- User interface features. Though most oxygen concentrators operate with same principles, the alarms, indicators, and device settings are variable. Oxygen concentrators should indicate, through alerts or alarms when: oxygen concentration is less than 82%; there is no oxygen flow; high/low pressure; power supply failure; or high temperature. Time meters that record cumulative hours of operation are also useful features.
- Patient Interface Consumables and Accessories. Delivering the oxygen from the concentrator to the patient requires outlet adaptors, oxygen tubing, replaceable (single use) nasal prongs or catheters (or oxygen masks for higher flows).
- Spare parts. Spare parts are generally NOT interchangeable between different types, models, brands of oxygen concentrators
- Training. In addition to appropriate clinical training for use of supplemental oxygen, technicians and engineers should perform regular maintenance and service checks. Some manufacturers include useful videos and instructions online for performance verification; routine maintenance and service checks; monitoring of concentration and outlet pressure; and repair and management of spare parts.
Special Considerations for Neonate/Pediatric Use
- Oxygen flow is extremely important to manage in order to not cause immediate or long-term health issues for neonates, especially premature or very small babies. Some oxygen concentrators are designated for use with newborns and have the ability to titrate down to very low flow rates (0.1-0.2 L/Min) Flowmeters and flow-splitters are important to manage flow for the safety of all patients, but especially for neonates. Concentrators with intermittent flow are unlikely to be suitable for oxygen therapy for newborns. Flowmeters should be capable of providing a minimum flowrate of 0.5 LPM and a maximum would depend on clinical need. Because some oxygen concentrators only provide flow down to 2 L/min, flow rates for neonate use might require accessories (flowmeters or flowmeter stands) that can titrate flow down to very low flow rates (0.1-0.2 L/min).
- Humidification. Consulting clinical guidelines based on the patient and the use is the most important consideration. The World Health Organization (WHO) guidelines indicate that humidification is NOT necessary when oxygen is used at low flow rates (up to 2 L/min) with nasal prongs or catheters in children younger than 5 years old. Humidification may be required if the oxygen bypasses the nose such as through nasopharyngeal catheters or tracheal tubes), which can be provided either through a humidification bottle provided by the manufacturer and connected between concentrator and patient breathing circuit.
- Blended Oxygen Gas. Premature babies and infants may require 30% oxygen to prevent oxygen toxicity; which often requires an oxygen-air blender device. However, such devices cannot be used with oxygen concentrators because the concentrators do not have sufficient pressure. For this reason, blended oxygen is typically provided through CPAP or ventilator devices to neonates. (See Buyers Guides for CPAPs)
VIA Global Health is committed to supporting health systems access affordable and appropriate medical products to improve the health in their communities. Products included in our Buyers Guides are available for purchase at VIA Global Health.
References and Acknowledgments
(1) NEST360° 2nd Edition Technical Report, February 2020;
(2) World Health Organization (WHO) Technical Specifications for Oxygen Concentrators 2015.
